Information

Reviewed by Dr Rohanti Ravikulan, MD
Information last reviewed 11/26/19
About
What is acid reflux?
Acid reflux, or gastroesophageal reflux disease (GERD), is a condition in which the stomach contents rise up through to the esophagus (food pipe), causing symptoms such as heartburn or regurgitation. GERD is the most common gastroenterological disorder in the US, with about 20% of Americans experiencing weekly symptoms. Everyone experiences GERD at some point in their lives and it is not always serious, but long-standing GERD can cause complications and needs to be evaluated.
Causes
What causes GERD?
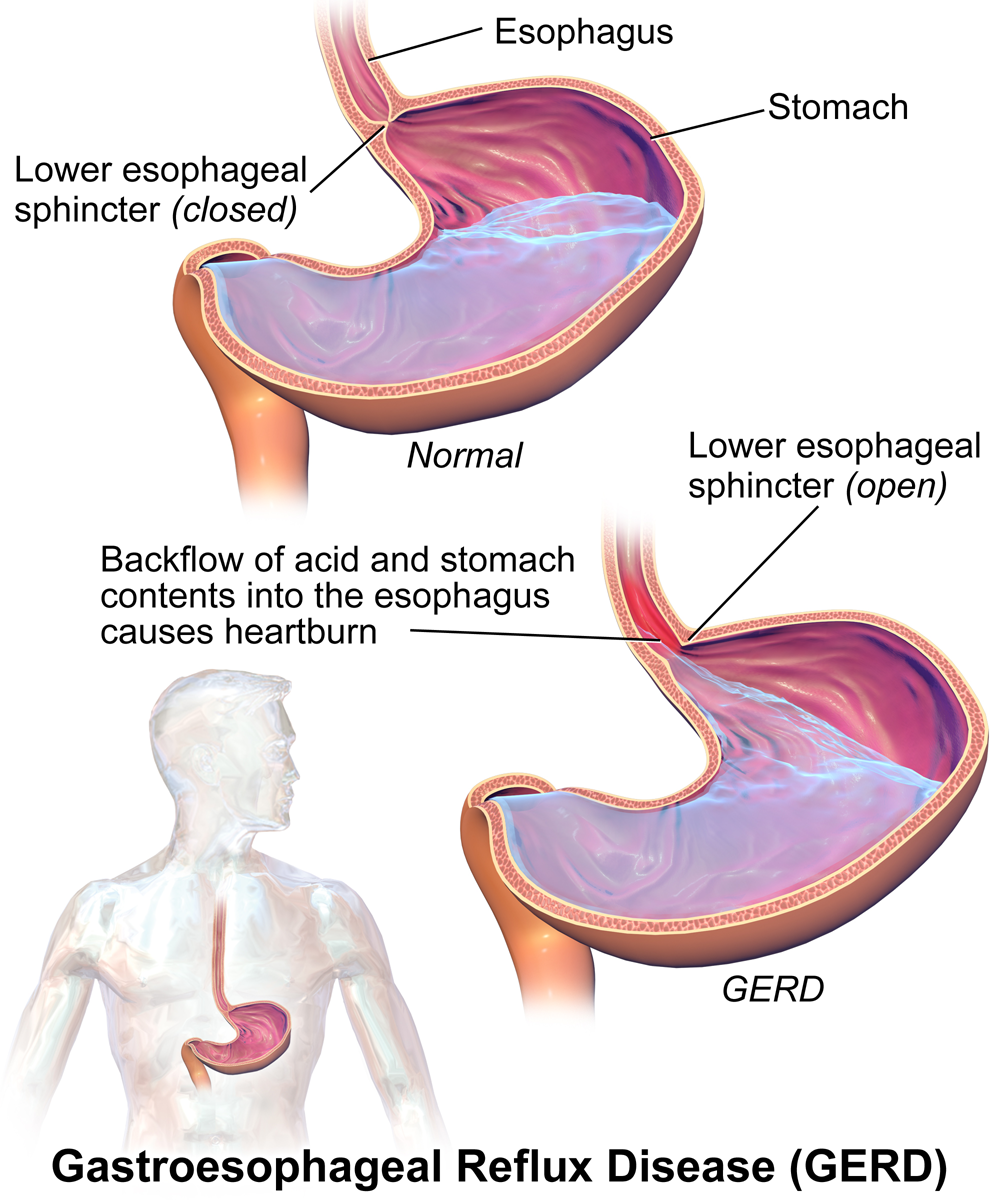
The part where the esophagus (food pipe) connects to the stomach is known as the gastroesophageal junction (GEJ). At this junction, is a sphincter, known as the lower esophageal sphincter (LES). The LES is essentially a circular band of muscle around the lower end of the esophagus that is constricted. This is shown in the diagram below.
As you can see, the constriction formed by the LES separates the esophagus from the stomach. In a healthy individual, the LES only relaxes to let food pass through from the esophagus to the stomach, and is closed at other times, preventing the gastric acid (stomach juice) from flowing back up the esophagus. The LES also occasionally relaxes to release the air trapped in the stomach, which leads to a burp or belch.
In individuals with GERD, the LES relaxes at the wrong time (not to let food pass or for a burp), leading to reflux of the stomach contents, causing symptoms like heartburn and regurgitation (when the contents come up all the way to the throat). In chronic cases of GERD, the constant backflow of the stomach acid irritates the esophagus, which can lead to inflammation and complications.
There are several causes of GERD, and include:
- Eating certain foods, such as fried and fatty foods (which delay stomach emptying), citrus fruits (which are acidic in nature), and spicy foods (which irritate the esophagus and stomach)
- Drinking certain beverages such as alcohol, coffee, and carbonated beverages which can increase gastric acid production and irritate the esophagus (food pipe) and stomach
- Eating large meals or eating very late at night which could delay the emptying of the stomach and cause reflux
- Smoking, which has a relaxing effect on the LES (since it is a muscle)
- Certain medications, such as anti-inflammatories and nitrates
- Obesity can increase the risk of reflux due to the excess belly fat pressing on the stomach
- Hiatal hernia, a condition where a portion of the stomach bulges up into the diaphragm
- Delayed emptying of the stomach due to conditions that cause the muscles of the digestive tract from functioning properly
- Pregnancy, where the hormones of pregnancy cause relaxation of the sphincter over the stomach, and the growing uterus pushes up on the stomach causing acid reflux
- Connective tissue disorders (conditions that affect the type of tissue that connects the structures in the body), such as scleroderma
Basically, acid reflux occurs when there is abnormal relaxation of the LES, which can occur due to or in addition to the following factors:
- increased acidity of the stomach acid
- delay in emptying of the stomach
- increased pressure on the stomach
- irritation of the stomach or esophageal (food pipe) lining
Symptoms
What are the symptoms of GERD
Common symptoms of GERD are:
- Heartburn, a burning sensation in the chest. This is the most common symptom of GERD. It usually occurs after eating and it may be worse at night. Some people may feel chest pain.
- Sour or bitter taste in the mouth due to regurgitation of the food
- Difficulty in swallowing or the sensation of a “lump” in the throat
- Bad breath
- Erosion of the teeth due to exposure to the stomach acid
If you are experiencing night-time GERD, some of the other symptoms you may have are:
- Persistent cough or a sore throat due to continued irritation of the throat
- Difficulty sleeping or disturbed sleep
- New-onset or aggravation of existing asthma if the regurgitated acid is breathed in
As mentioned earlier, long-standing acid reflux can lead to complications due to inflammation caused by the constant backflow of stomach acid. Some of these complications are:
- Esophageal ulcers: This is caused by the stomach acid wearing away the lining tissue in the esophagus (food pipe), leading to an open sore. Esophageal ulcers can cause pain or difficulty during swallowing and they can bleed.
- Esophageal strictures: This is the narrowing of the esophagus. It occurs because of damage to the esophagus lining which causes scar tissue to form. The build-up of scar tissue narrows the pathway, causing obstruction and difficulty swallowing.
- Barrett’s esophagus: Constant exposure of the esophageal tissue to stomach acid causes damage, which causes the tissue to undergo structural change. These changes can eventually lead to esophageal cancer.
Diagnosis
Upper Endoscopy
In this technique, your doctor inserts a thin, flexible tube (endoscope) with a camera down your throat, to see the inside of your esophagus (food pipe) and stomach. In cases of mild reflux, there may not be any abnormalities seen, but if there is any inflammation or damage, this can be visualized. A sample of the tissue, known as a biopsy, may also be taken to test for complications like Barrett’s esophagus (where the tissue has changed in structure).
pH Monitoring
This technique involves placing a monitor in your esophagus (food pipe) to see how often and for how long stomach acid regurgitates. The monitor could be a thin, flexible tube (known as a catheter) that is passed through your nose into the esophagus, or it could be a clip that is placed in your esophagus through endoscopy and passes in your stool after a couple of days. The monitor is connected to a wearable computer that is placed around your shoulder or waist (depending on the type of device, which can be wireless).
Manometry
This test measures the rhythmic movements or contractions of the muscles in the esophagus during swallowing. It is helpful to identify any conditions that are related to improper functioning of the nerves and muscles, leading to acid reflux.
X-ray
For this test, you would be asked to drink a solution or swallow a pill (most commonly containing the metal, barium) following which an X-ray of the upper digestive system is taken. The barium highlights the outline of the digestive tract which allows the health practitioner to see any narrowings (strictures) in the esophagus or other structural problems in the pathway that may be causing acid reflux.
Treatment
Lifestyle changes
If you only have occasional and/or mild reflux, there are some lifestyle changes you can adopt that may alleviate your symptoms. These include:
- Avoiding foods and beverages that may trigger reflux
- Establishing and maintaining a healthy weight: Excess fat puts pressure on the stomach which causes reflux
- Elevating your head when you are lying down: This put the upper part of your esophagus higher than your stomach, making it harder for the acid to flow back up
- Not lying down immediately after you eat: You should wait for at least two to three hours after eating before you lie down
- Stopping smoking: Smoking has a relaxing effect on the LES which increases the reflux
- Chewing your food thoroughly and eating slowly: Swallowing large morsels quickly can cause the muscles in the esophagus to spasm
Medical therapy
Both over-the-counter and prescription medications are available for the treatment of GERD. Your doctor will usually recommend lifestyle changes and over-the-counter treatments as the first step. If you don’t see allevitation of your symptoms in a few weeks, prescription medications are likely to be the next step.
The commonly used over-the-counter medications for GERD are:
- Antacids: Antacids are medications that neutralize the acid in your stomach. Examples include Gelusil, Gaviscon, and Pepto-Bismol. Taking antacids can give you rapid relief but they will not heal any inflammation or damage that has been caused to the esophagus.
- H-2-receptor blockers: These medications reduce the production of stomach acid. They are not as quick-acting as antacids but they decrease acid production for up to 12 hours, so provide longer relief. Examples of H-2-receptor blockers include ranitidine (Zantac), nizatidine (Axid), famotidine (Pepcid AC) and cimetidine (Tagamet HB).
- Proton Pump Inhibitors (PPIs): These medications block acid production in the stomach and they are much stronger than H-2-receptor blockers in reducing stomach acid. Because they have such a powerful effect on stomach acid production, they allow the esophageal tissue to heal. Most PPIs are only available on prescription but some are available over-the-counter. These include omeprazole (Losec), lansoprazole (Prevacid 24HR), and esomeprazole (Nexium).
The prescription medications for GERD are similar to the over-the-counter medications, except that they are stronger. These include:
- H-2-receptor blockers (prescription-strength): These include the same medications as those mentioned in the over-the-counter section (ranitidine, famotidine, and nizatidine), but are of a higher strength.
- Proton pump inhibitors (PPIs, prescription-strength): These include the medications from the over-the-counter section (omeprazole, lansoprazole, and esomeprazole) in higher strengths, as well as others such as rabeprazole and dexlansoprazole.
- Baclofen: This medication works by decreasing the frequency of LES relaxations.
Surgical therapy
Most cases of GERD can be treated with medical therapy. However, in some instances, where long-term therapy is needed or medical therapy does not provide relief, surgical therapy may be the best option. The most common surgical procedure is fundoplication. This is a technique where the top part of the stomach is wrapped around the lower end of the esophagus and sewed there. This is done to tighten the muscle in the area and prevent backflow of stomach acid. This is a minimally invasive procedure (laparoscopy), where a thin tube with a camera is inserted through a small incision on the abdomen and the surgery is performed using the feed from the camera.
There are several other surgical techniques that may be used and your surgeon will recommend the options that are best suited to your condition.
Comparison Table
Q&A
Yes, PPIs are safe to be taken during pregnancy. The FDA has classified omeprazole in particular as a “category C” drug (animal studies show risk but human studies are inadequate or lacking or no studies in humans or animals), based on old data. But several recent studies have shown that omeprazole, like all other PPIs, are safe in pregnancy.
For the occasional heartburn, taking an antacid should provide immediate relief. You should also avoid lying down for two to three hours after a meal. However, if the frequency of your heartburns increase, and lifestyle changes and over-the-counter medications are not providing relief, you should consult a health practitioner.
Some studies suggest that certain PPIs like omeprazole and dexlansoprazole may be more effective than others, however, the evidence is inconsistent. In general, prescription-strength PPIs are more effective than over-the-counter forms purely because of the difference in doses.
There is some evidence that stress is associated with an increased risk of GERD. Stress can release certain substances within the body that affect our muscles and other organs. This can lead to abnormal relaxation of the lower esophageal sphincter (LES), causing stomach acid reflux.
Indigestion, or dyspepsia, is a term given to a spectrum of causes that lead to pain or discomfort felt in the stomach, usually after eating. It could be due to several reasons, which include overeating, eating greasy foods or foods that disagree with you. Heartburn is a very specific symptom, characterized by a burning sensation in the chest due to the backflow or regurgitation of stomach acid and stomach contents. Heartburn may also be a symptom of indigestion. The main difference between indigestion and GERD is that GERD always involves a backflow of stomach acid, but in indigestion, there may or may not be stomach acid reflux.
When the stomach acid reflux is short-term, there is generally no damage to the esophageal lining, and this is known as non-erosive GERD (where the tissue is not eroded by the stomach acid). In long-standing cases of GERD where the esophageal lining is repeatedly in contact with the stomach acid, the tissue undergoes damage, and this is known as erosive GERD (where the tissue is eroded by the stomach acid). In short, if non-erosive GERD is prolonged and untreated, it can turn into erosive GERD.
If your heartburn isn’t responding to over-the-counter PPIs after a week or two, you should consult a health practitioner who is likely to prescribe a higher dose of PPIs and/or evaluate the cause of your heartburn, based on which the best treatment options for you can be recommended.
If you feel heartburn, you have stomach acid reflux. And though acid reflux is the main problem in GERD, the major difference is the frequency of acid reflux. Occasional acid reflux in response to certain foods occurs in everyone and is not abnormal. But if you have acid reflux more than two or three times a week and/or the other symptoms of GERD, it means you are more likely to have GERD
Disclaimer: This is not medical advice. You and your physician will determine if and how you should take any medication prescribed to you following a medical consultation.
- Dent J, El-Serag HB, Wallander MA, Johansson S. Epidemiology of gastro-oesophageal reflux disease: a systematic review. Gut 2005; 54:710.
- Nebel OT, Fornes MF, Castell DO. Symptomatic gastroesophageal reflux: incidence and precipitating factors. Am J Dig Dis 1976; 21:953.
- Kahrilas PJ, Shaheen NJ, Vaezi MF, et al. American Gastroenterological Association Institute technical review on the management of gastroesophageal reflux disease. Gastroenterology 2008; 135:1392.
- Katz PO, Gerson LB, Vela MF. Guidelines for the diagnosis and management of gastroesophageal reflux disease. Am J Gastroenterol 2013; 108:308.
- Kahrilas PJ. Gastroesophageal reflux disease. JAMA 1996; 276:983.
- Song EM, Jung HK, Jung JM. The Association Between Reflux Esophagitis and Psychosocial Stress. Dig Dis Sci 2013; 58:2
- Chen L, Chen Y, Li B. The efficacy and safety of proton-pump inhibitors in treating patients with non-erosive reflux disease: a network meta-analysis. Nature 2016.
- Zhang C et al. Effectiveness and Tolerability of Different Recommended Doses of PPIs and H2RAs in GERD: Network Meta-Analysis and GRADE system. Sci Rep. 2017; 7: 41021.













Quick and discreet
I ordered Azithromycin tablets for chlamydia treatment, received it next day in a brown discreet pack, and cheaper than all other pharmacies, can't ask for more
Jordan McCann